When Millimeters Matter: Advanced Resection of a Giant Meningioma

A male patient in his mid-30s presented with nearly a year of progressively debilitating headaches accompanied by profound fatigue and reduced functional stamina. As symptoms escalated and began to affect daily activity, diagnostic imaging revealed a large intracranial mass consistent with a giant meningioma - a benign, dural-based tumor whose size and mass effect can create urgent neurologic risk despite non-malignant pathology.
Given the tumor’s substantial volume and the degree of compression on adjacent brain structures, the patient was referred for urgent neurosurgical evaluation at Adventist Health Glendale, where he was assessed by neurosurgeon Dr. Yaser Badr.
Clinical challenge: "Giant" meningioma
Meningiomas arise from the meninges and often grow slowly, allowing symptoms to remain subtle until the lesion reaches a size that disrupts normal intracranial dynamics. "Giant" meningiomas - commonly used to describe tumors >5 cm - can produce symptoms through mass effect and increased intracranial pressure. Depending on location, patients may experience:
- Persistent or progressive headaches
- Seizures
- Focal neurologic deficits (weakness, sensory changes, coordination impairment)
- Cognitive or personality changes
- Visual or speech disturbances
In these cases, surgical strategy must balance two equally critical goals: maximal safe resection and preservation of neurologic function.
Millimeters matter - particularly when the tumor abuts vascular structures, cranial nerves, and eloquent cortex.
Operative approach: technology-enabled precision with experienced judgment
Dr. Badr led a carefully planned resection designed to optimize the extent of removal while protecting surrounding brain tissue and critical neurovascular anatomy. Complex meningioma surgery benefits from a program built for high-acuity neurosurgical care, integrating tools and teams that support safety and precision throughout the case, including:
- Advanced neuronavigation ("GPS for the brain") to align preoperative imaging with real-time anatomy and guide tumor boundary identification.
- High-definition operative microscopy to enhance visualization during delicate microdissection
- Intraoperative neuromonitoring to support functional preservation during critical phases of resection
- Specialized neuro-anesthesia and neurocritical care to optimize hemodynamics, brain relaxation, and postoperative neurologic surveillance
- Coordinated perioperative imaging and neuroradiology support to inform decision-making and follow-up planning
While technology strengthens intraoperative precision, outcomes in giant meningioma surgery ultimately depend on surgeon expertise - particularly the ability to anticipate anatomic complexity, manage vascular risk, and make time-sensitive intraoperative decisions that protect neurologic function.
Multidisciplinary continuity from diagnosis to recovery
Adventist Health’s Neuroscience Institute model emphasizes integrated care across the full continuum, aligning surgical expertise with specialized postoperative management. For complex intracranial tumor cases, this often includes:
- Dedicated neuro-ICU nursing and advanced practice support
- Close neurologic monitoring and complication prevention pathways
- Rehabilitation services when functional recovery support is indicated
- Longitudinal follow-up for surveillance imaging and symptom monitoring
- This coordinated framework helps accelerate recovery, reduce fragmentation, and support a safe transition back to daily life.
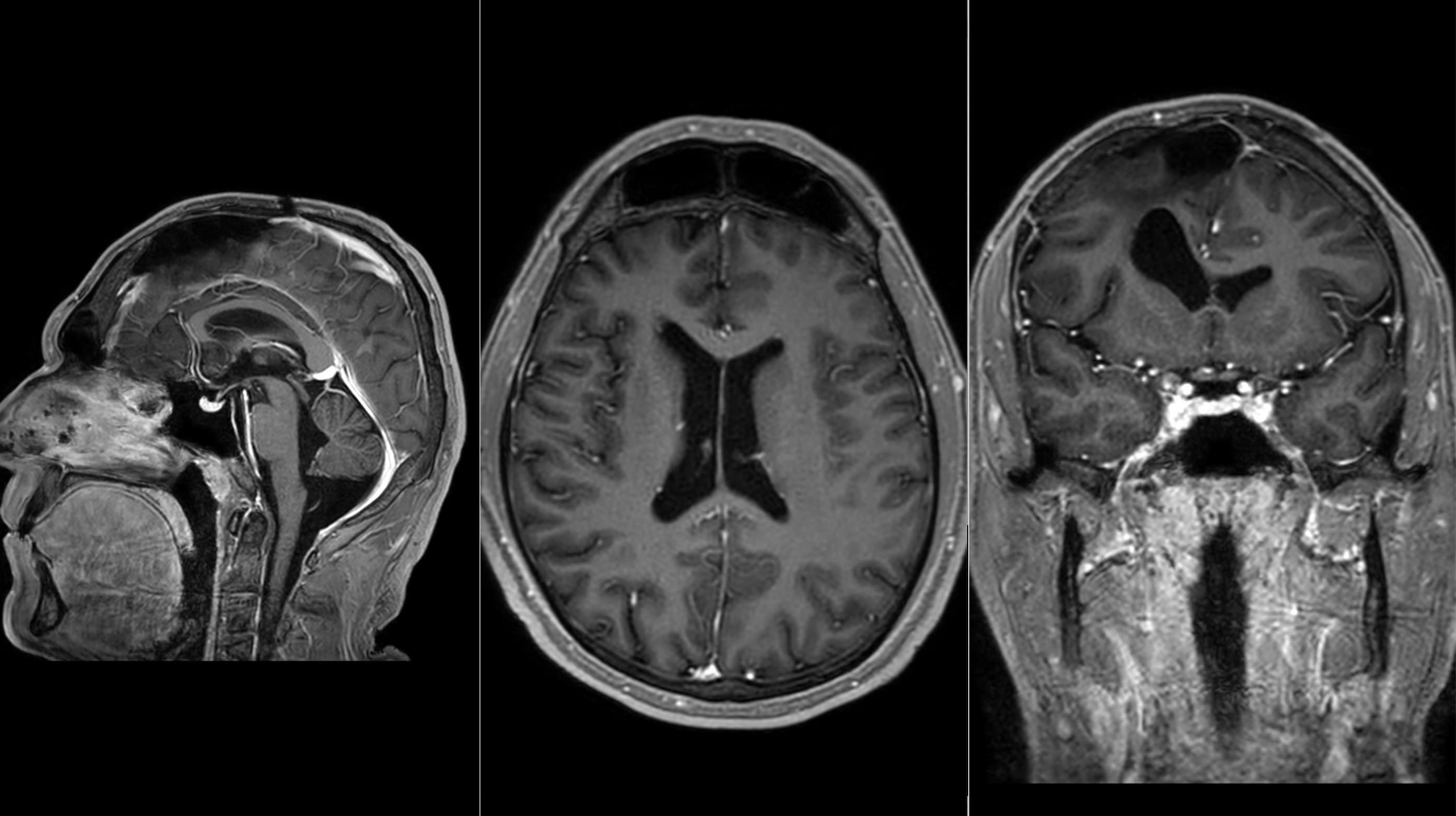
Postoperative scan after resection of a giant meningioma, showing the surgical result and successful tumor removal, and restoration of intracranial space.
Restoring quality of life
Following successful resection, the patient experienced meaningful improvement in the symptoms driving functional decline. Over time, he was able to resume higher levels of activity and return to the routines and relationships most important to him - reflecting the core objective of modern neurosurgery: not simply removing a tumor, but protecting independence and restoring quality of life.
Why this case matters
Giant meningiomas represent a high-complexity subset of benign brain tumors - often operable, but not routine. This case underscores the advantage of receiving care in a setting where experienced subspecialty neurosurgery is paired with precision-guided operative technology and a high-reliability neurocritical care ecosystem.
In a region where patients have choices, Adventist Health Glendale’s Neuroscience Institute continues to demonstrate readiness for complexity - delivering meticulous neurosurgical planning, advanced intraoperative capability, and multidisciplinary recovery support under the leadership of expert clinicians like Dr. Badr.