Breast Saved Against All Odds Thanks to Tumor Board Collaboration on Invasive, Aggressive Tumor

A 48-year-old postmenopausal patient triple-negative breast cancer (TNBC) progressed into one of the most advanced and complex cases ever treated by the hospital's Breast Tumor Board.
The patient initially discovered a lump under her left arm in March 2020 while showering. Dismissing it as a minor issue, she waited to seek medical help. By the end of the year, the mass had grown to the size of a grapefruit. When she finally sought care at a major Los Angeles-area academic hospital, the diagnosis was blunt: high-grade invasive ductal carcinoma, triple-negative, and no possibility of preserving the breast.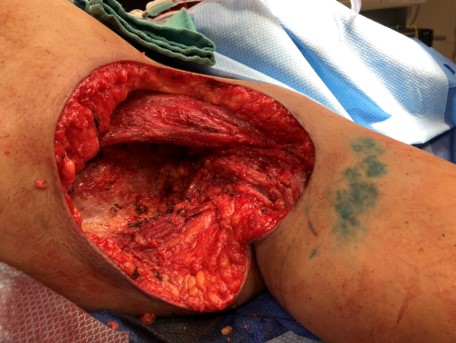
However, the patient was not ready to give up hope. That search for options led her to Dr. Dennis Holmes, breast surgeon and Medical Director of the Sam and Grace Carvajal Comprehensive Breast Center at Adventist Health Glendale.

Dennis R Holmes, MD
"[The patient] presented with a massive, infected tumor that had grown over 20 months," Dr. Holmes recalled. "Her tumor occupied the left axillary region and had grown to the size of a basketball. She was in constant pain, unable to lower her arm, and at significant risk for life-threatening complications."
A core biopsy confirmed the aggressive nature of her cancer:
- Histology: High-grade invasive ductal carcinoma
- Biomarkers: ER-negative, PR-negative, HER2/neu-negative
- Ki-67: 70%, indicating a very high proliferative index
- Genetic testing: Negative
- Imaging:
- Ultrasound: 13 x 12 x 13 cm axillary mass
- CT Chest: 15 x 15 x 12 cm breast/axillary mass with multiple abnormal nodes; no distant metastases
- MRI: 13 x 13 x 14 cm mass with skin involvement and nodal disease
- CT Abdomen/Pelvis: No distant metastases
Due to the extent of disease and infection, Dr. Mihran Shirinian, Tumor Board oncologist, immediately initiated aggressive neoadjuvant therapy, beginning with intravenous antibiotics to control infection, followed by a tailored chemotherapy and immunotherapy protocol:
- Neoadjuvant chemotherapy
- Keytruda (pembrolizumab) + Adriamycin/Cytoxan, q3 weeks x 4 cycles
- Keytruda + Taxol, q3 weeks x 4 cycles
- Adjuvant chemotherapy (completed December 2023)
- Keytruda, q3 weeks x 8 months
- Xeloda (capecitabine), 2 weeks on/1 week off for 8 months
The tumor responded dramatically, shrinking rapidly. "We saw substantial necrosis and resolution of the infection," Dr. Shirinian said. "That response made surgery both safer and more feasible."
Still, the surgical risks remained extraordinarily high. Given the tumor's involvement of critical vascular structures in the axilla,Dr. Edward Samourjian, a vascular surgeon, joined the Tumor Board for preoperative planning. "The tumor was adjacent to major arteries and nerves," he explained. "There was a serious risk of catastrophic bleeding or permanent nerve injury. We had to be extremely precise."
Dr. Peter Ashjian, a plastic and reconstructive surgeon, was also consulted early to plan a closure using a latissimus dorsi flap, given the anticipated defect size. "We harvested skin, fat, and muscle from her back to close the cavity created by the tumor resection," Dr. Ashjian said. "Time was of the essence. Any further delay would have made surgery nonviable."

Peter Ashjian, MD
On the day of surgery, the team worked in synchronized precision. The mass was successfully removed, major vascular structures preserved, and the patient’s breast reconstructed. Upon waking, her first question was whether her breast had been saved. "Being able to say yes—that we preserved her breast—was one of the most fulfilling moments of my career," said Dr. Holmes.
Today, the patient is in complete remission. She continues routine follow-ups, grateful for what she calls her "second chance at life."
"This was in the top 1% of cases in terms of complexity," said Dr. Shirinian. "Without the shared expertise of every specialist on the Tumor Board, we could not have achieved this outcome."
Key Takeaways for Referring Physicians
- Triple-negative breast cancer (TNBC) requires urgent, aggressive multidisciplinary care.
- Early referral can significantly improve outcomes, especially when breast preservation is a priority.
- Adventist Health Glendale's Breast Tumor Board offers integrated surgical, medical, vascular, and reconstructive expertise in a single setting—avoiding the need for patients to navigate disjointed, multi-institutional care.
To refer a patient or consult with a member of the Tumor Board, please contact the Sam and Grace Carvajal Comprehensive Breast Center at Adventist Health Glendale at 818-630-8680.
