Adventist Health Glendale Introduces Pulsed Field Ablation for Atrial Fibrillation
Adventist Health Glendale’s Cardiology Program has adopted Pulsed Field Ablation (PFA) as a new energy modality for catheter ablation in patients with atrial fibrillation (AFib), further advancing its role as a regional center for complex electrophysiology (EP) care. This non-thermal technology offers a tissue-selective approach to atrial ablation with the potential to improve safety, efficiency, and patient experience.
“Adventist Health Glendale continues to invest in the most advanced cardiac technologies available, ensuring that our patients receive the safest, most effective therapies close to home,” said Harry Balian, MD, Medical Director of Cardiovascular Services at Adventist Health Glendale. “Bringing Pulsed Field Ablation to our community reflects our commitment to world-class innovation and evidence-based care.”

John McKenzie, MD, Cardiac Electrophysiology and Cardiology
How Pulsed Field Ablation Works
Catheter ablation is a cornerstone of contemporary AFib management. Antiarrhythmic drug therapy typically achieves rhythm control in only ~50% of patients, whereas catheter ablation offers success rates exceeding 80% in appropriately selected individuals.
Traditional ablation techniques rely on thermal energy — radiofrequency (heat) or cryotherapy (cold) — to achieve lesion formation. In contrast, PFA delivers short bursts of high-voltage electrical energy, producing irreversible electroporation of cardiomyocytes. This results in controlled cell death while largely sparing non-cardiac tissues.
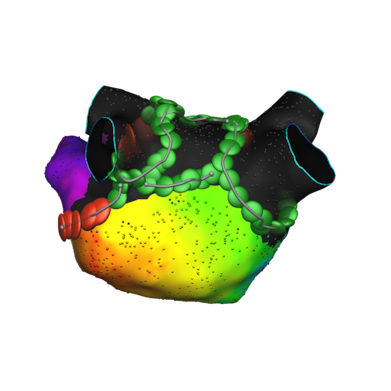
During PFA, a catheter is advanced via venous access (most commonly femoral) to the left atrium. Once positioned around the pulmonary veins, the Affera™ system delivers precisely timed electrical pulses that create microscopic pores in atrial myocytes, achieving pulmonary vein isolation while minimizing injury to adjacent structures such as the esophagus, phrenic nerve, and pulmonary veins themselves.

The system’s all-in-one catheter allows for tissue-selective pulsed field energy or traditional radiofrequency (heat-based) energy from the same device during a procedure.
“The core elements of the procedure — vascular access and three-dimensional electroanatomic mapping — are unchanged,” explained John McKenzie, MD, Cardiac Electrophysiology and Cardiology, who performed the first PFA procedure at Adventist Health Glendale. “What is new is the therapeutic modality. PFA is highly tissue-selective, more efficient, and in many cases offers a favorable safety profile compared with conventional thermal energy.”
Program Development and Technology Selection
The introduction of PFA at Adventist Health Glendale was preceded by a multi-year evaluation and readiness process led by Dr. McKenzie, including comparison of available PFA platforms and alignment of clinical, anesthetic, and operational protocols.
“As an electrophysiologist, a substantial proportion of my practice is devoted to catheter ablation for atrial fibrillation,” said Dr. McKenzie. “Point-by-point thermal ablation has served our patients well for many years. However, this new energy source allows us to treat AFib more efficiently, with a meaningful safety advantage for selected populations.”
Adventist Health Glendale has adopted the Affera™ mapping and ablation system by Medtronic, which Dr. McKenzie characterizes as the most advanced of the current generation of PFA technologies.
“PFA represents a paradigm shift in how we approach atrial fibrillation ablation,” he noted. “Its tissue selectivity significantly reduces the risk of collateral injury to nearby organs. Because therapy delivery is rapid, procedure times are often less than two hours, compared with the traditional two- to three-hour window for thermal ablation. This translates to less anesthesia exposure, more same-day discharge, and accelerated recovery.”
Dr. McKenzie anticipates that PFA will become the default energy source for AFib ablation. “This is the future of catheter ablation,” he said. “Once centers transition to PFA, there is little reason to revert to older energy platforms for most AFib cases.”
Early Patient Experience
Early PFA cases at Adventist Health Glendale demonstrate clinically relevant improvements in symptom burden and quality of life:
-
Younger athletic patient: A man in his mid-30s, an avid soccer player, experienced AFib episodes reliably triggered by high-intensity exertion, effectively sidelining him from the sport. After shared decision-making regarding catheter ablation, he elected to undergo PFA, a technology he was already aware of. He ambulated within hours post-procedure, resumed light activity within several days, and returned to running approximately one week later. He has since resumed competitive play without recurrent symptomatic AFib.
-
Older patient with symptomatic paroxysmal AFib: A 65-year-old man with hypertension had recurrent AFib episodes lasting 12–48 hours, associated with palpitations and fatigue rated around 6/10 in severity. He was intolerant of antiarrhythmic medication. He underwent PFA while in active AFib. Symptomatic improvement was evident within two weeks, and by three months he reported a marked change in day-to-day functioning, with the ability to liberalize activity and resume previously avoided triggers such as coffee.
“These cases illustrate the practical impact of PFA,” said Dr. McKenzie. “Beyond the technology, the goal is durable rhythm control, symptom reduction, and restoration of patients’ functional status.”
“Introducing PFA aligns with our mission to deliver world-class tertiary services and life-bettering care, grounded in current evidence and guideline-directed practice,” added Dr. Balian. “We are committed to partnering with referring physicians to select the most appropriate candidates and optimize longitudinal outcomes.”
